Paraffin Wax Bath Treatments
Aching Feet That Won’t Warm Up? If you suffer from cold feet, discoloured toes, or painful chilblains, a Paraffin Wax Bath treatment might be exactly what you need. Many patients come in feeling frustrated after trying everything from wool socks to hot water bottles, only to find their feet are still icy cold.
Fortunately, there’s a soothing, effective solution.
What Is a Paraffin Wax Bath?
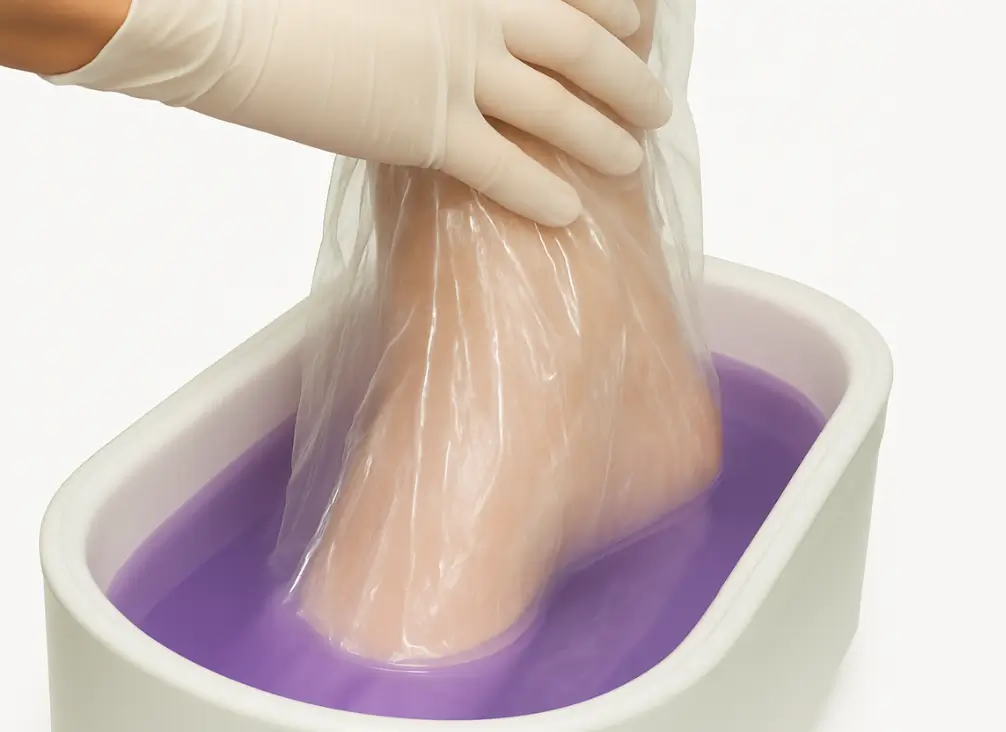
A Paraffin Wax Bath is a therapeutic treatment where your feet are gently immersed in warm, melted paraffin wax. The wax forms a cocoon around your feet and gradually transfers heat deep into the tissues over a 20-minute session.
The wax used is specially designed to retain warmth while remaining at a safe, comfortable temperature. For hygiene, our podiatrist places a protective plastic liner between the skin and the wax.

Who Can Benefit From a Paraffin Wax Bath
If you experience any of the following, you might find relief with a paraffin wax treatment:
-
Persistently cold feet, even indoors
-
Discolouration or pain due to poor circulation
-
Chilblains or painful red sores on the toes
-
Arthritis-related joint stiffness or discomfort
-
Raynaud’s symptoms triggered by cold
-
Stiff feet after long periods of inactivity
Key Benefits
Paraffin wax treatments offer a range of therapeutic effects:
-
Deep, lasting warmth for cold, numb feet
-
Improved circulation by dilating small blood vessels
-
Pain relief in muscles and joints
-
Softer, healthier skin from moisturising effects
Safe, Comfortable and Relaxing
Paraffin wax therapy uses low, controlled temperatures, making it a safe and gentle option for most people. It’s commonly used to help with poor circulation, chronic cold feet, or joint stiffness. While the treatment is generally well-tolerated, it is NOT recommended for those with open wounds, active skin conditions (like eczema or psoriasis flare-ups), or significant sensory loss in the feet (such as in severe diabetes).
Podiatrists recommend paraffin wax not just for temporary relief, but as part of a broader approach to improving quality of life in individuals with long-term foot and lower limb concerns. Sessions are quick, non-invasive, and deeply soothing.
If you’ve tried everything to warm your feet and still suffer discomfort, don’t give up. This simple, comforting treatment could make a real difference. Let warmth support your circulation, reduce joint pain, and help you feel normal again.

Have Questions About Podiatry?
We’re here to make it simple. Whether you’re dealing with ongoing foot pain or just unsure if podiatry is right for you, we’re happy to guide you — no pressure, just clear answers.









